Pressure cooker in rural general practice
A primary care survey report shows that general practices in rural Otago and Southland are feeling the pressure, and are, compared to their urban counterparts, more likely to struggle to retain workforce, fill gaps and therefore provide care for the community they live in.
Here is the Primary Care Survey November 24 Full Analysis Report
Here is the WellSouth Primary Care Survey Summary Nov 2024
CEO of WellSouth, the primary health organisation for Otago and Southland, Andrew Swanson-Dobbs says the WellSouth Primary Care Survey was established to understand the challenges facing primary care providers in the Southern region directly from them.
“While this is only the second survey of its type, we can see ongoing pressure and constraints, most acutely felt in our small, rural general practices.”
WellSouth has been surveying general practices and pharmacy since COVID-19 monthly check-ins. The new six monthly, more comprehensive survey launched in April 2024 covers pressures on workforce, capacity, and funding.
“From the first April survey to the next, we have seen little relief or change to pressures for general practice”, says Mr Swanson-Dobbs.
“Across the survey themes, rural practices are most strained. Workforce shortages were more common, and many described the impact of limited staffing on their ability to sustain service delivery, innovate, or maintain staff wellbeing.”
WellSouth has the largest geographic region of any PHO in Aotearoa New Zealand, with almost half of the general practices on the WellSouth network, rural.
‘General practitioners’ remain the most frequently reported shortage in rural areas where shortages are nearly triple those in urban settings. While the total number of respondents reporting shortages remained steady, shortages in Clutha and Gore increased.
Mr Swanson-Dobbs says this reflects the difficulty recruiting GPs in rural areas.
“Fewer people are willing to live and work rurally, and it unsustainable for rural practices to offer higher salaries to attract staff. There is a lack of on-site doctors, and an increasing reliance on locums. Staff shortages limit appointment availability, impacting service delivery, and in some cases, make it difficult for practices to stay financially sustainable. Some report that a single resignation could significantly tip the balance,” he says.
“Many staff, especially owners and senior staff, are working long hours, staying late, and taking on extra duties to keep up with demand. They do this because they care about their patients and want them to have good access to quality care.”
“High demand against an insufficient workforce leads to closed books or restricted enrolments,” he says.
“All of this plays a part in how patients and staff interact with each other, creating pressure cookers with patients unhappy and abusive to staff, which in turn affects job satisfaction and customer service.”
“We urgently need to address the rural shortfall and support those community’s health needs,” says Mr Swanson-Dobbs.
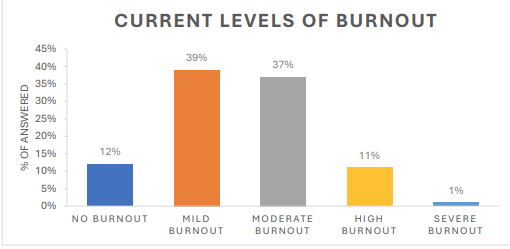
The survey shows that overall, mood and morale have remained largely stable since April 2024 across the urban and rural practices, with a slight shift towards being more positive, with only 11% rating ‘Poor’ or ‘Very Poor’ compared with 15% on April 24. Despite this, feedback shows that most general practice staff are experiencing mild to moderate burnout.
One respondent said:
“Burnout for many people needs a solution higher than just the practice support. The practice can't fix the problems with the rest of the health system that cause the stress and moral injury. But the team is very supportive of each other - the main reason we are able to continue functioning.”
Mr Swanson-Dobbs says, “We must address the system and persistent under-funding of primary care. In terms of system change, our respondents talked about nurse pay parity, greater support and resources for primary care due to the workload pushed back from secondary care. We must ease the administrative burden from non-contact time, and review appointment structures and ways to address patient expectations.”
Mr Swanson-Dobbs commends practices that are adapting to pressures across rural and urban.
“Triage improvements, expanded nursing roles, and telehealth are offering partial relief. However, acute demand continues to take priority over proactive care, and financial barriers prevent implementation of effective solutions.
“A system-wide approach is needed, with targeted funding and workforce investment to ensure primary care and in particular our rural general practices and staff is not just sustainable but is an attractive sector to work in offering high job satisfaction.”
More about the survey
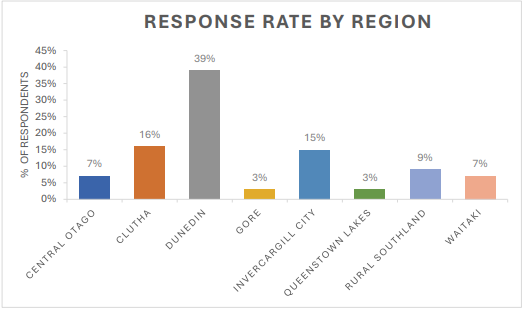
This survey had 143 responses, an increase from the 119 responses received in April 2024, and with more respondents from rural parts than the previous survey. Respondents represented the diversity of our primary care workforce, including general practitioners, nurses, administrators, practice managers, and pharmacists. The number of distinct practices was 24, representing 30% of all WellSouth practices. However, this is likely an underestimation, as 71% of respondents did not disclose their practice name. Respondents were not required to provide their practice name to ensure anonymity, making it unclear exactly how many practices were represented.
Rural vs Urban Representation
For the purpose of this survey, the definition of Rural or Urban was based on the Geographic Classification for Health, as this is consistent with whether they receive rural funding or not. Rural responses increased from 37% in April to 45% in November, now closely matching the overall network distribution of 43% rural practices. This suggests growing engagement from our rural-based practices.
WellSouth’s network consists of 79 general practices, 34 of which (43%) are rural, collectively serving 337,000 enrolled patients as of January 1, 2025. These practices are (at time of last data collection) supported by 336 general practitioners, 31 nurse practitioners, 422 nurses, and a range of non-clinical kaimahi, including administrators and practice managers.
View more news