Tēnā koutou katoa
Welcome to the end of another week! Peter Ellison and I attended the start of our inaugural Pae Ora – Healthy Futures Primary Care Leadership course last week in Dunedin. It warmed my heart to meet 19 of our general practice, Māori provider and Pacific provider clinicians and managers from across the whole district, all keen to laern more about leadership and equity in the primary care space. Feedback has been really positive so far. We will be evaluating the impact of the course, and I am hopeful we will be able to provide more people this opportunity in the future.
The main focus for today’s update is the Winter Wellness Check programme we launched this week. Someone said to me recently, “We can’t do everything but we can always do something”. We will be evaluating if this version of ‘doing something’ impacts on better equitable health outcomes for some of those people in our communities most at risk of getting crook this winter.
Last night I met with other primary care clinical leaders from across the South Island, Te Wai Pounamu, and Chiquita Hansen, the Regional Wayfinder for Te Whatu Ora. She talked about her new role of commissioning primary and community care services for Te Wai Pounamu, and opportunities to work together. Chiquita was the CEO of THINK Hauora, a PHO in the Manawatu area and has primary care in her bones. I am also part of the Te Wai Pounamu Clinical Leaders group, where the clinical leaders from hospital and specialist services across the South Island and primary care clinical leaders (myself and Anna Wheeler from Timaru representing the primary care group) meet to chart our course for regional clinical leadership. I do think this work will bear fruit for an integrated approach to how we do things in the South, as the reforms slowly unfold.
Key points today:
-
Winter Wellness Check
-
Aotearoa Immunisation Week
-
Planned Care Update -- Letters to patients on surgical waiting lists longer than 4 months
-
Health Reforms - National Clinical Networks
-
Advanced Dermatoscopy Course
-
Introducing our Clinical Advisors
-
GPNZ Primary Care Clinical Digest – May 19, 2023
-
Covid updates
What’s new
Winter Wellness Check
The Winter Wellness Check launched Monday 22 May and will run until Friday 30 June 2023. Our aim is to help provide additional resources to help practices to support patients most at risk of getting unwell to stay healthy over winter.
In the few days since the programme launched we have had great feedback coming through from practices.
We would like to provide further information and few clarifications, including:
-
Thalamus Dashboard
-
Access and Choice practices and the Winter Wellness Check
-
Care Plans
-
Online Drop-in Q&A webinars
Thalamus Dashboard - Asthma
We wanted to take this opportunity to clarify that Thalamus data is pulling only patients with asthma + a prescription of an inhaled corticosteroid in the last 12 months.
The purpose of the Winter Wellness Check is to focus on those who have the most need/are most likely to deteriorate over winter. Therefore, we feel it makes sense to focus on those who have asthma + a prescription of an inhaled corticosteroid in the last 12 months.
However, the claiming form does not restrict to these criteria. If there is a patient who has asthma, who has not been prescribed an inhaled corticosteroid in the last 12months, and you think this programme is appropriate for them (i.e. there is a significant risk of them deteriorating over winter) then you can offer this check to them.
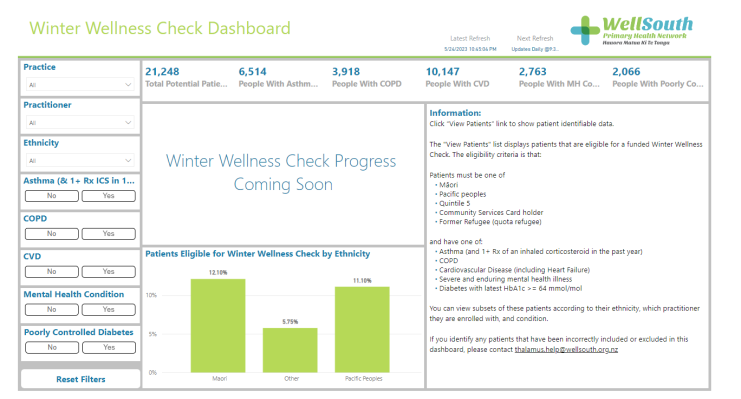
Just remember that there is not enough funding for all your eligible patients to receive this check so it is important to prioritise those who will benefit most. 5000 Winter Wellness Checks equates to about 1.5% of our population, and you can use this as a rough guide for your practice’s numbers. The Thalamus dashboard can help you identify your eligible patients, for MedTech practices. Once the Halcyon portal is up and running, you will also get a daily update of your patients who have already had a check, by ethnicity. This will show in the ‘Winter Wellness Check Progress Coming Soon’ space below:
Toku Oranga-Access and Choice
While Health Improvement Practitioners (HIPs), Health Coaches, and Community Support Workers (CSW) cannot complete a Winter Wellness Check, they can play an important role in ensuring the patient stays well. The Tōku Oranga (Access & Choice) team are working to ensure they can problem-solve ideas with patients to keep their homes healthy over winter.
Health Coaches can also support by proactively contacting patients eligible for a Winter Wellness Check and problem-solving barriers to attendance.
For practices without Access & Choice, useful information on how to support patients to keep a healthy home this winter can be found here: https://www.southernhealth.nz/living-well/healthy-homes (further useful links at the bottom of this webpage).
Care Plans – Patient Action Plans, Acute Plans, Personalised Care Plans, Advance Care Plans – What’s in a name??
The Winter Wellness check will provide an opportunity to create discuss, initiate or update care plans for your patients with long-term conditions. It can get confusing about which is which.
Patient Action Plans are patient facing. They are what the person takes away with them to have at home to remind them what to do if they become unwell. Its written in collaboration with the person and they use it to look after themselves in the early phases of becoming unwell, and it directs them as to when they need to seek further help. An asthma action plan is a great example of this. Find templates to print and use on our Winter Wellness Plans webpage.
Acute Plans (or acute care plans) are provider facing. They are part of the suite of on-line, electronic care plans that sit in HealthOne. These include Acute Plans, Personalised Care Plans, and Advanced Care Plans. Shared Care Planning is designed to allow community, primary and hospital health care providers working together to proactively manage and plan care with patients who have complex health needs.
For the Winter Wellness Check we want you to create or update the Acute Plan sitting in HealthOne for the person you are working with. It is a place to put key relevant clinical information about the person if they end up in ED, seeing another practice or after-hours provider, or if the ambulance arrives, to help that clinical team care for the person. It is a great place to put usual O2 sats for people with COPD, usual body weight for someone with heart failure, etc.
If you are not familiar with this part of HealthOne, our Winter Wellness Plans webpage has been updated with a step by step Guide to Acute Care Plans, which has screenshots of where to find the care plan in HealthOne. This is very helpful – click the link and check it out if you haven’t created an Acute Plan in HealthOne for a while.
Evaluation of Winter Wellness Checks
This is a new initiative and we want to understand if what we all feels makes sense to do, actually impacts on patient outcomes over the winter illness period. Rather than create an onerous claim form full of mandatory tick boxes, we have taken a ‘high trust’ approach of letting you all know what we are trying to achieve, with guidance of what we would like you to do as part of the Winter Wellness Check.
We will be assessing what elements of the check have been done, and the impact of having a Winter Wellness Check on outcomes for patients. Much of this data we can collect without asking you to tick boxes on the claim form. The only piece of information we can’t collect electronically without asking you is whether the person was given a patient action plan. This is why we are asking this on the Halcyon Portal claim form, when that gets up and running in a week or two. Hence why we are asking you to keep NHI numbers of people you have provided a Winter Wellness Check for, and whether they were given a patient action plan during the check. The form will prepopulate for most of the other fields:
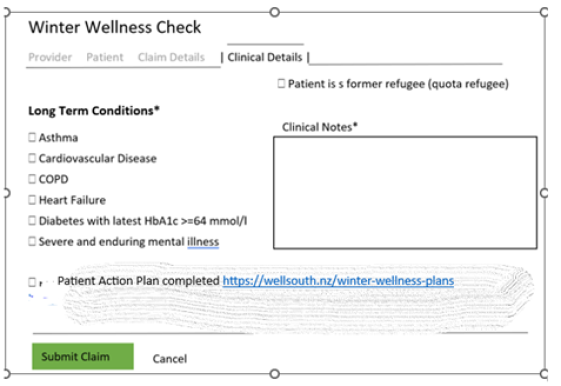
We will also be seeking some provider and patient feedback on what the process was like at the end.
Thanks for your cooperation.
Questions?
If you have questions about the Winter Wellness Check or need assistance with care plans, please contact your Practice Relationship Manager.
Drop-In Sessions:
We have held a couple of Q+A webinars to assist with the Winter Wellness Checks, and will hold another one in a couple of weeks , full details and links to join that webinar is below. We will soon post the link to last night’s webinar which provides a short overview of the programme as well.
Thursday 8th June @ 12pm - Click here to join the meeting
Meeting ID: 470 894 314 961
Passcode: CzX5uy
Aotearoa Immunisation Week 29 May to 4 June
As you may be aware, Te Whatu Ora - National Public Health Service are working on a national immunisation campaign called Aotearoa Immunisation Week. This is planned for the period of Monday 29 May - Sunday 4 June. There is funding available to general practices, community pharmacy and community providers to promote immunisations. Additional Workforce support or extended hours, outreach services, whānau manaakitanga packages and clinic decorations or accessories can all be funded. While this work is focused on next week, indications from the Regional Wayfinder, Chiquita Hansen, last night, was that any activities that promote immunisations during June will be fundable, as long as invoiced before the end of June.

Planned Care Update – Letters to patients on surgical waiting lists longer than 4 months
You may have heard in the media today that Te Whatu Ora will be sending letters to patients next week (31 May) who have been waiting on the surgical (ESPI5) waiting list for longer than 4 months. This is a national process. In Te Whatu Ora Southern, patients who have been waiting longer than 4 months, but have recently been contacted by the hospital services regarding their appointment won’t be contacted. About 2500 patients will receive the letter. The letter seeks to update contact details, and provide information. It is not a letter to remove people from the list, but some people may be unsettled by it and seek reassurance from their primary care team as a result.
We have been provided with information for primary care providers, template letter for your information, and a set of FAQs that may help your team answer questions from patients.
We appreciate that this may cause you additional work and if you have particular concerns or would like to discuss, please contact me.
Health Reforms - National Clinical Networks
Earlier this week, new National Clinical Networks were launched by Te Whatu Ora. Primary Health Care organisations were not involved in this initial launch, and GPNZ is writing a letter to Te Whatu Ora about ensuring engagement with primary care at all levels as the networks are developed and partnership through their ongoing mahi.
The following email from Te Whatu Ora outlines this initiative and provides a link to the video if you are interested. When the expressions of interest for the Co-leads come out we will let you all know.
“Thank you to those of you who were able to attend Tuesday’s Introducing National Clinical Networks event. If you weren’t able to make it, you can watch a recording of the event. Please also cascade this to other kaimahi who may be interested.
The recording includes:
-
An address by Health Minister Ayesha Verrall outlining about her vision for the networks
-
A panel discussion, which included the Minister and the co-chairs of the National Clinical Networks Governance Group
-
A question and answer session with members of the in-person audience
National Clinical Networks
The establishment of new national clinical networks, with common operating approaches and membership from professional disciplines across hospital and primary care, will support clinicians across the system to lead and drive change through the development of national standards and models of care. They will support the delivery of consistent service quality and outcomes, including the reduction of access and equity gaps, across the country. Te Pae Tata identifies the establishment of regional and national networks as a key step in removing unwarranted variations in access to care, waiting times and clinical practice.
Next Steps
We will continue to provide more information on the establishment of the networks. Our next milestone will be to open the Expression of Interest process for co-leads of the first tranche of networks within the new few weeks.
Ngā mihi
Mary Cleary-Lyons
Interim Group Manager – Clinical Networks
Hospital and Specialist Services”
waea pūkoro: +64 27 222 5843
Upcoming training and webinars
Southern Nurses Conference - Save the date

Date: 13 - 14 October 2023
Location: Ōtepoti, Dunedin
We are pleased to announce our upcoming Southern Nurses Conference for 2023.
More details will be provided about the conference agenda and speakers in the coming months, but for now please save the date. Registrations will open in July 2023.
Advanced Dermatoscopy Course
Date: 29 - 30 July 2023
Location: University of Auckland, City Campus
Skin Cancer Symposiums invite you to the upcoming Certificate of Advanced Dermatoscopy course at the University of Auckland, City Campus on 29 – 30th July 2023.
The course has been endorsed by The Royal New Zealand College of General Practitioners (RNZCGP) and has been approved for up to 25 CME credits for CPD purposes.
Check out the course flyer for full details here.
Other general information
Introducing our clinical advisors
This week we are introducing another one of our clinical advisors at WellSouth. Please feel free to contact Aisha if you have an issue or idea relating to their area.
Dr Aisha Paulose, Clinical Advisor
I was appointed as the first Clinical Advisor for WellSouth in 2019 and its great to have a team of us working together now.
I am a huge advocate of our specialty and I believe that the more of us front line clinicians working in leadership roles, the better for Primary care and our patients.
I am a born and bred Londoner and graduated from University College London and Royal Free Medical School in 2004. I qualified as a GP, attaining MRCGP in 2009 and worked in Kent and London in multiple roles before emigrating to New Zealand in 2015.
After spending 2 years travelling and working in practices across the South Island, I settled in Murihiku, Southlands and achieved Fellowship in 2016.
I live in the peace and quiet of Winton Surrounds with my husband and 4 year old son (the pic attached is the view from my dining table)
I worked in various education streams with the UK RCGP from 2008 and attained a Post Graduate Certificate of Education.
Upon arriving in New Zealand I have picked up the equivalent educational roles that I held in the UK.
I am a GP at Winton Medical Services which has a great embedded collegial and training culture.
In my Clinical advisor role for WellSouth my key role is placing and providing teaching and support for PGY2s in CBA scheme and well as some GP CME.
I work with the RNZCGP as Lead Medical Educator for the Southlands GPEP1 programme and a Medical Educator for facilitating learning groups for GPEP2/3s.
I have been involved in supervising Medical Students, Nurse and Paramedic Practitioners in the UK and also NZ. I also hold various other roles such as; Clinical editor for Southern health pathways, Educator for Otago Medical School and running education sessions for MobileHealth.
Aisha.Paulose@wellsouth.org.nz

The view from Aisha’s window
GPNZ Primary Care Clinical Digest – May 19, 2023
In this issue:
-
Immunisation Update - May 18 2023
-
Webinar – Planning for Palliative Care Services in Aotearoa: What our Population Data Tells Us
-
Proposal to Fund Candesartan with Hydrochlorothiazide Tablets for High Blood Pressure
-
Listening to Families – Website / YouTube Resource
-
Just Breathe Conference: June 17-18 2023 Auckland
-
ACC Strategic Clinical Advisor – Māori Health Position
-
Telehealth Consultation – MCNZ
-
Reminder: IFAC 3rd Asia Pacific Conference on Integrated Care (APIC3), Sydney November 13-15 2023
-
Updates for Pharmacists in General Practice weeks ending May 12 and May 19 2023
-
Top Weekend Viewing
Read the full update here.
Covid-19 updates
Southern Numbers
Covid numbers reported continue to bobble along in between 100-230 reports daily over the last couple of weeks, but I’m guessing many people aren’t reporting their positive Covid tests given the number of people I know who have it! I am still a Novid, but am becoming more rare (and possibly tempting fate by saying this!).
Figures for the last month below:
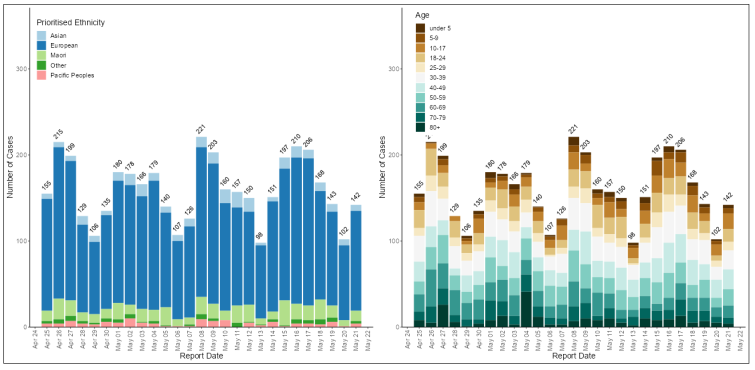
What beyond 30 June for Covid funding?
Next week I’m hoping we will know what will happen with Covid funding beyond 30 June, and as soon as we know we will pass this on.
So I hope you all have the opportunity to have some down time this weekend. And that you get to enjoy the first King’s Birthday weekend in most of our living memories next weekend!
Ngā mihi nui
Carol